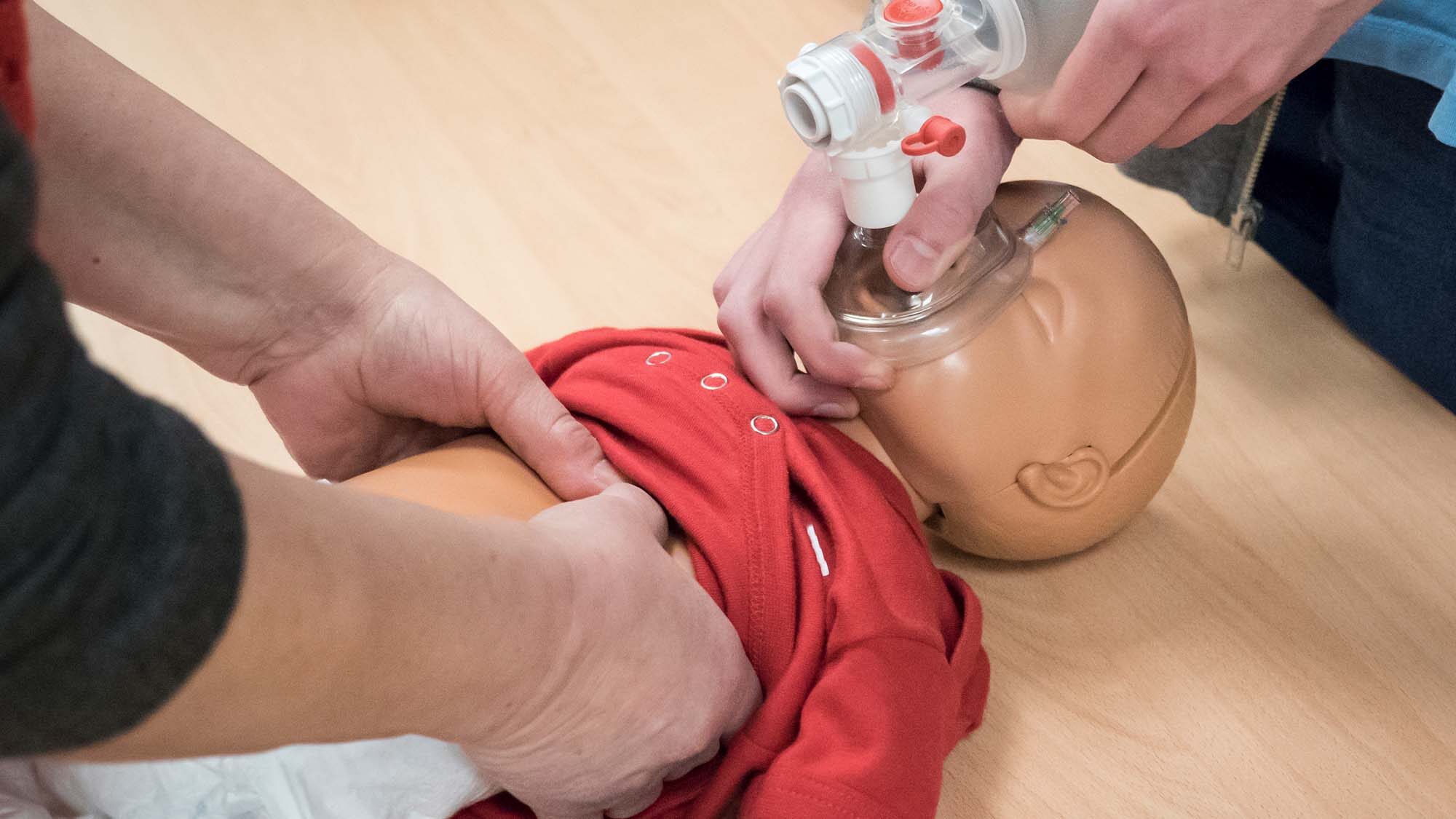
Thank you for making our Grand Opening a huge success!
Last Wednesday, we hosted 60 people in our new Critical Care Training Center facility. We had representatives from Kaiser Hospital, Olympia Medical Center, Holly Cross Hospital, Northridge Medical Center and Mission Community Hospital as well as college representatives from West Coast University, Concorde College, CSULA and CSUN. We are excited to serve this group of medical providers and educators. Thank you!

Now That’s Funny!
 Submit your funny cartoon, picture or story for a chance to win a $20 gift certificate if your image is chosen for our next newsletter. This week’s comic relief was submitted by Richard, and RN from Valley Presbyterian Hospital.Submit your funny to support@acls123.com by Friday, September 28th for the next issue of our newsletter.
Submit your funny cartoon, picture or story for a chance to win a $20 gift certificate if your image is chosen for our next newsletter. This week’s comic relief was submitted by Richard, and RN from Valley Presbyterian Hospital.Submit your funny to support@acls123.com by Friday, September 28th for the next issue of our newsletter.
Every week we’ll be taking an in-depth look at a medical issue or health syndrome. This week we bring you Sick Sinus Syndrome; over the next few weeks we’ll bring you topics like
Ulysses Syndrome
Turner’s Syndrome
Korsakoff Syndrome
Adams-Stokes Syndrome
EDUCATION
Cushing’s Syndrome
Definition
Cushing’s syndrome occurs when your body is exposed to high levels of the hormone cortisol for a long time. The most common cause of Cushing’s syndrome, sometimes called hypercortisolism, is the use of oral corticosteroid medication. The condition can also occur when your body makes too much cortisol.
Too much cortisol can produce some of the hallmark signs of Cushing’s syndrome — a fatty hump between your shoulders, a rounded face, and pink or purple stretch marks on your skin. Cushing’s syndrome can also result in high blood pressure, bone loss and, on occasion, diabetes.
Treatments for Cushing’s syndrome can return your body’s cortisol production to normal and noticeably improve your symptoms. The earlier treatment begins, the better your chances for recovery.
Symptoms
The signs and symptoms of Cushing’s syndrome vary. Common signs and symptoms involve progressive obesity and skin changes, such as:
- Weight gain and fatty tissue deposits, particularly around the midsection and upper back, in the face (moon face) and between the shoulders (buffalo hump)
- Pink or purple stretch marks (striae) on the skin of the abdomen, thighs, breasts and arms
- Thinning, fragile skin that bruises easily
- Slow healing of cuts, insect bites and infections
- Acne
Women with Cushing’s syndrome may experience:
- Thicker or more visible body and facial hair (hirsutism)
- Irregular or absent menstrual periods
Men with Cushing’s syndrome may experience:
- Decreased libido
- Decreased fertility
- Erectile dysfunction
Other signs and symptoms include:
- Fatigue
- Muscle weakness
- Depression, anxiety and irritability
- Loss of emotional control
- Cognitive difficulties
- New or worsened high blood pressure
- Glucose intolerance that may lead to diabetes
- Headache
- Bone loss, leading to fractures over time
When to see a doctor
If you’re taking corticosteroid medications to treat a condition, such as asthma, arthritis or inflammatory bowel disease, and experience signs and symptoms that may indicate Cushing’s syndrome, see your doctor for an evaluation. Even if you’re not using these drugs and you have symptoms that suggest the possible presence of Cushing’s syndrome, contact your doctor.
Causes
Cushing’s syndrome results from excess levels of the hormone cortisol in your body. Your endocrine system consists of glands that produce hormones, such as cortisol, that regulate processes throughout your body. These glands include the adrenal glands, pituitary gland, thyroid gland, parathyroid glands, pancreas, ovaries (in females) and testicles (in men).
Your adrenal glands produce a number of hormones, including cortisol. Cortisol plays a variety of roles in your body. For example, cortisol helps regulate your blood pressure and keeps your cardiovascular system functioning normally. It also helps your body respond to stress and regulates the way you convert (metabolize) proteins, carbohydrates and fats in your diet into usable energy. However, when the level of cortisol is too high in your body, you may develop Cushing’s syndrome.
The role of corticosteroids
Cushing’s syndrome can develop from a cause that originates outside of your body (exogenous Cushing’s syndrome). Taking corticosteroid medications in high doses over an extended period of time may result in Cushing’s syndrome. These medications, such as prednisone, have the same effects as does the cortisol produced by your body.
Your doctor may prescribe corticosteroids to treat inflammatory diseases, such as rheumatoid arthritis, lupus and asthma, or to prevent your body from rejecting a transplanted organ. Because the doses required to treat these conditions are often higher than the amount of cortisol your body normally needs each day, the effects of excess cortisol can occur.
People can also develop Cushing’s from injectable corticosteroids — for example, repeated injections for joint pain, bursitis and back pain. While certain inhaled steroid medicines (taken for asthma) and steroid skin creams (for skin disorders such as eczema) are in the same general category of drugs, they’re generally not involved in Cushing’s syndrome unless taken in high doses.
Your body’s own overproduction
The condition may also be due to your body’s own overproduction of cortisol (endogenous Cushing’s syndrome). This may occur from excess production by one or both adrenal glands, or overproduction of the adrenocorticotropic hormone (ACTH), which normally regulates cortisol production. In these cases, Cushing’s syndrome may be related to:
- A pituitary gland tumor. A noncancerous (benign) tumor of the pituitary gland, located at the base of the brain, secretes an excess amount of ACTH, which in turn stimulates the adrenal glands to make more cortisol. When this form of the syndrome develops, it’s called Cushing’s disease. It occurs much more often in women and is the most common form of endogenous Cushing’s syndrome.
- An ectopic ACTH-secreting tumor. Rarely, when a tumor develops in an organ that normally does not produce ACTH, the tumor will begin to secrete this hormone in excess, resulting in Cushing’s syndrome. These tumors, which can be noncancerous (benign) or cancerous (malignant), are usually found in a lung, pancreas, thyroid or thymus gland.
- A primary adrenal gland disease. In some people, the cause of Cushing’s syndrome is excess cortisol secretion that doesn’t depend on stimulation from ACTH and is associated with disorders of the adrenal glands. The most common of these disorders is a noncancerous tumor of the adrenal cortex, called an adrenal adenoma. Cancerous tumors of the adrenal cortex are rare, but they can cause Cushing’s syndrome as well. Malignant tumors of the adrenal glands (adrenocortical carcinoma) are rare, and sometimes produce excess cortisol. Occasionally, benign, nodular enlargement of both adrenal glands can result in Cushing’s syndrome.
- Familial Cushing’s syndrome. Rarely, people inherit a tendency to develop tumors on one or more of their endocrine glands, affecting cortisol levels and causing Cushing’s syndrome.
Read the entire article including Complications and Treatments here.
NEWS
 How has the nursing and EMS industry changed during your career?
How has the nursing and EMS industry changed during your career?
Did you wear uncomfortable starched uniforms? Aprons? Caps? One nurse reported that she was always called Nurse, never by her given name. And she and her colleagues were required to formally address patients–Mrs. Mr., Miss. Of all of the changes during your career, which do you find the most surprising, helpful or funny? What these nurses had to say at their 50 year reunion.
Virtual Emergency: Simulator Trains for Childbirth Emergencies
By Jeannine Aquino, Photo by Peter Holderness
 “OK, push at the next contraction, OK? And push . . . very good,”? said a resident physician to his patient Noelle, a 39-year-old mother about to deliver her fourth child.
“OK, push at the next contraction, OK? And push . . . very good,”? said a resident physician to his patient Noelle, a 39-year-old mother about to deliver her fourth child.
The baby’s head peeks out, but the shoulders get stuck. The baby’s heart rate drops steadily. More nurses and another resident rush in to help.
“Push hard, deep breath, Noelle! Push, push, push, push!”?
After the baby slips out, the team quickly brings the infant’s heart rate back to normal.
“You have a baby girl,”? said one nurse to the mother, who wore a green gown, tan socks and a blank stare. “Congratulations!”?
The happy “mother”? is actually a life-sized computerized patient simulator used as a training tool by the obstetrics staff at Columbia St. Mary’s Hospital Milwaukee. The pregnant mannequin allows the medical center’s labor and delivery unit to practice emergency delivery situations without the real emergency. Read the entire article here.

Green coffee bean extract diet: Fat burner or lame buzz?
By Elisa Zied, R.D.
On a recent episode of “The Dr. Oz Show,” green coffee bean extract — a supplement created from green (unroasted) coffee beans — was touted as a “fat burner that helps women lose weight.”
Oz tested the effects of the extract on 100 women. Half were given 400 mg of green coffee bean extract 30 minutes before breakfast, lunch, and dinner for two weeks; the other half were given a placebo. Participants were told to maintain their regular diets and to keep a food journal. The women who took the extract lost two pounds on average, while the placebo group lost an average of one pound
Since the episode aired, green coffee bean extract has become one of the most searched terms online. It’s mostly available in pill form, but earlier this summer Starbucks added it as part of a new line of low-calorie drinks, which are being promoted as a “boost of natural energy.”
However, few published studies have examined the extract’s effects on weight loss — and none over the long term.
In a recent small, 22-week study, researchers gave 16 overweight adults low doses of green coffee bean extract (350 mg, twice a day), high doses of the supplement (350 mg, 3 times a day), or a placebo (3 times a day) for 6 weeks each with a 2-week break of not taking the pills between sequences. Subjects were encouraged to be physically active, but no dietary changes were recommended.
Results of the study, funded by Applied Food Sciences, Inc. (a company that manufactures green coffee bean extract) and published in the journal Diabetes, Metabolic Syndrome and Obesity, found that subjects who took the extract lost about 18 pounds on average — more than 10 percent of their body weight. No adverse side effects were noted. Read the entire article here.